Enhanced care coordination programs, also called "wraparound," empower families caring for a child or teen with significant behavioral health needs, including mental health and substance use disorders.
Wraparound programs have helped hundreds of Granite State families navigate complex systems as they face a child's intensive behavioral health challenges. However, private insurance does not cover these services, creating barriers for Granite State families and costing taxpayer dollars unnecessarily.
Senate Bill 498 would help more Granite State families access the care they need, regardless of their insurance type.
Learn More about Wraparound Programs
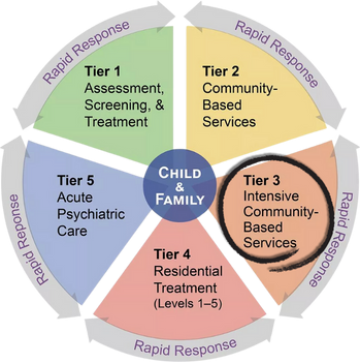
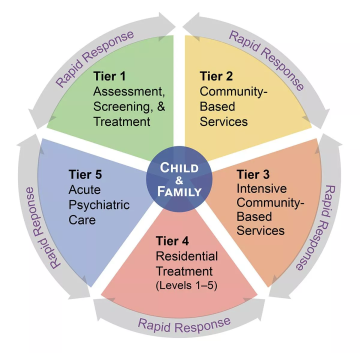
New Hampshire’s Children's System of Care for behavioral and mental health was designed with wraparound programs as its Tier 3 - Intensive, Community-Based Services. They are the Granite State's version of a proven youth- and family-centered planning and care coordination process.1 These programs serve families who have tried less intensive treatments and/or have complex situations requiring them to be involved in more than one “system” (e.g. juvenile justice, child protection, special education).
Wraparound programs help families clarify their strengths and needs. They then bring together a team to develop and implement a plan alongside them. The team can include the child, family, professional service providers, and other trusted adults.
There are three distinct wraparound programs in New Hampshire:
- FAST (Families and Systems Together) Forward wraparound for ages 5-21
- Early childhood wraparound for birth to 5
- Transitional Enhanced Care Coordination (TrECC) for youth in need of or transitioning out of residential treatment
Learn More About The Private Health Insurance Coverage Gap
While wraparound is included as part of Medicaid, it is unfortunately not covered by private health insurance corporations. This means Granite State families who purchase health insurance through their employer or the marketplace face significant barriers or may not be able to access these critical services.
To ensure access, stopgap measures currently allow some acutely ill children to become eligible for Medicaid through a special program, but not until their mental health challenges become severe.
Other families have had their wraparound care covered with taxpayer general fund dollars.
These extra steps have unnecessarily delayed appropriate care for children and teens while their struggles intensified.
Take Action
Learn the Facts - SB 498 Mythbusters
MYTH #1: This is a Medicaid program.
It’s not. FAST Forward, the program that provides wraparound, serves every child in New Hampshire regardless of their insurance type. The system of care in New Hampshire exists for every single child in this state. Right now private carriers refuse to pay for their own members accessing these services, so New Hampshire taxpayers are currently picking up the tab.
MYTH #2: This bill will raise premiums.
At most, this assessment costs 24 cents per member per month. Families are already paying nearly $7,000 a year out of pocket for private coverage that provides zero support during a pediatric mental health crisis. Twenty-four cents.
This program is cost saving. Since 2014, when New Hampshire rolled out this program, the Department of Health and Human Services (DHHS) has experienced a 28% reduction in inpatient hospitalization expenses. 28%! This was millions of dollars. Because kids are being served in their community instead of costly institutions.
Let's also consider what's already happening: when private carriers refuse to cover these children and their condition worsens, the kids get pushed onto Medicaid — which New Hampshire taxpayers fund at 50 cents on every dollar. When children get community-based care early, they don't end up in hospitals.
So that 24 cents, even that is a stretch. Realistically, this bill could actually drive costs down.
MYTH #3: This bill would require changing several laws.
Not true. While any bill can be subject to a legal challenge, even if meritless, this bill contains an important provision that protects it: a severability clause. This means that, even if insurance carriers tried to challenge this in court, the bill is built to withstand it. If one piece of the bill were ever struck down, the rest of the law stays standing. So the core assessment framework would be preserved. We know this because it is modeled on New Hampshire's vaccine association, which has never seen a successful legal challenge.
MYTH #4: The right people haven't been working on this.
This issue has been studied exhaustively. There have been three formal processes examining this exact problem: the Insurance Department's Behavioral Health Advisory Committee, an interim legislative study committee convened in 2022 specifically to pursue a non-legislative solution to SB 70, and the SB 411 study committee in 2024. Non-legislative solutions were also pursued last year, after the House removed the policy from their version of the Budget in Committee of Conference. In all of these meetings, industry experts have been present, participating and reporting progress on contracts that have never materialized. House members have also been involved and even sit on the Insurance Department’s Behavioral Health Advisory Committee. The groundwork has been laid. What hasn't happened is action.
MYTH #5: Providers haven't been coming to the table.
The two non-profit organizations delivering FAST Forward were actively in documented conversations with insurance carriers in 2024. Insurance carriers claim the providers haven’t given them the patient data they need to build the billing infrastructure needed to cover FAST Forward. But the reason patient data hasn't been shared isn't stonewalling — it's HIPAA, state law, and provider policies around confidentiality. They legally cannot share a child's clinical file with an insurance company that has made no commitment to pay for their care.
And here’s what the insurance carriers aren’t saying: Insurance companies analyze risk as part of their billion-dollar business models. You’d be shocked to know the amount of information they’re keeping on you to predict the costs associated with your current and future health conditions. So, they already know which of their members have been hospitalized for mental health crises. They know which families are filing outpatient claims. They know which of their patients suddenly has dual insurance because they now qualify for Medicaid. The idea that they don't know who these kids are is not credible.
MYTH #6: FAST Forward providers should have been billing insurance all along.
In every Department of Health and Human Services contract, there's a standard clause called the payer of last resort. It means: if private insurance doesn't pay, the state does. Private carriers have routinely denied Fast Forward claims, saying they don't cover these services and that the providers are not in their network. So the state has been paying — every time, for every child. Senate Bill 498 fixes this by ensuring carriers finally contribute their fair share instead of passing the cost onto taxpayers.
MYTH #7: This bill can't apply to self-funded insurance plans.
New Hampshire's private insurance market is roughly split — about half fully insured plans, and half self-funded plans. Here's why that matters: state laws around mandating benefits apply to fully insured plans, but not self-funded ones. So a standard insurance mandate would only reach half the market.
But the Supreme Court has clearly established that while states cannot mandate benefit designs for self-funded plans, they can impose indirect economic burdens — like surcharges or assessments — on health plans. Because an assessment is a cost of doing business rather than a directive on how to structure a benefit plan, it is a legitimate tool to reach self-funded plans.
That's exactly what Senate Bill 498 does. The assessment model captures both self-funded and fully insured plans — the entire private insurance market in New Hampshire. No loopholes. No carve-outs.
Share Your Story
Will you share your experience to help support insurance coverage for enhanced care coordination in NH? Stories are powerful tools that can be shared with lawmakers and the public to influence policy change. New Futures can help you develop effective ways to share your story.
- Have you, a loved one, a client/patient, etc. either benefitted from or struggled to access youth behavioral/mental health care?
- Do you have experience with enhanced care coordination, or "wraparound", also known as FAST (Families and Systems Together) Forward, early childhood wraparound, or Transitional Enhanced Care Coordination (TrECC)?
Spread the Word: Advocacy Brief & Social Media
Need help? Contact Wendy Chase (Community Engagement Coordinator) for help taking action or Emma Sevigny (Senior Policy Director, Children's Behavioral Health) with policy questions.
About the Bill
- Protect taxpayers by preventing state general funds from subsidizing private health insurance corporations.
- Require private health insurance companies to help pay for these mental health services, creating a partnership between public and private insurers.
- Allow Tier 3 of the Children’s System of Care to work as intended for the first time.
- Help New Hampshire children get needed care, no matter what type of insurance they have.
- Contribute to more Granite State children and youth access the right care at the right time.
Bill Status
Interim Study: Not moving forward this session.
May 26: The Committee of Conference met and failed to reach an agreement on HB 1323, ending its progess this session. New Futures will not stop fighting for children with private health insurance who deserve the same access to mental health services as anyone else.
May 14: The House of Representatives non-concurred with the Senate amendment to HB 1323, which includes components of SB 498, and requested a Committee of Conference to negotiate.
May 14: The House of Representatives voted 188-164 to adopt the Committee recommendation of Interim Study, effectively stalling the bill for this year. Later in the day, the House of Representatives made a motion to reconsider the bill, but the reconsideration vote failed, 183-162. Late in the evening, the Senate attached components of SB 498 to a House Bill, HB 1323, and passed it. Because the bill was amended in the Senate, it returns to the House for concurrence.
May 6: The House Commerce and Consumer Affairs Committee voted 14-4 to recommend that the bill's progress be halted and for the issue to be studied before the next legislative session. This issue has already been considered extensively by New Hampshire legislators, and non-legislative solutions have never come to fruition.
Earlier in 2026
April 28: A subcommittee of the House Commerce and Consumer Affairs Committee held a work session to further discuss the bill.
March 26: The full Senate approved the committee's recommendation as part of the consent calendar, meaning the bill was not debated on the floor and state senators used a voice vote to weigh in on it together with a group of other bills.
March 19: As the bill includes a fiscal note, it was considered in the Senate Finance Committee. The committee waived a second hearing and unanimously recommended the bill "ought to pass".
March 5: The full Senate agreed to move the bill forward on a unanimous voice vote as part of the consent calendar.
February 18: The committee voted 4-1 to recommend the bill as “ought to pass” to the full Senate, with Senators Regina Birdsell, Pat Long, Suzanne Prentiss, and David Rochefort in favor of the bill, and Senator Kevin Avard opposed.
February 11: The Senate Health and Human Services Committee held a public hearing. We are incredibly grateful to the many advocates who were in attendance. There were even two articles in the Concord Monitor that highlighted advocate stories and the importance of this bill.
2025 Legislation
Senate Bill 128 was similar to 2026's SB 498. The bill received unanimous support in the Senate Health and Human Services Committee, the Senate Finance Committee, and in the full Senate. The language from the bill was added to the Senate's version of the state budget, but it was removed during Committee of Conference negotiations with the House of Representatives. You can learn more at our archived webpage.
2024 Legislation
Senate Bill 411 originally sought to address the care coordination coverage gap, but was amended to instead create a committee to study emergency mental health services for youth in New Hampshire, leaving the problem unsolved. You can learn more at our archived webpage.
You can learn more about how New Hampshire's legislative process works on our About the Legislature webpage, or take one of our advocacy trainings. If you'd like to hear about the bill's progress, you can sign up for automated updates from the NH Legislature here.